In the past year, we’ve seen a tremendous number of positive changes to synchronous telemedicine in 3 areas:
- Flexible Delivery Models
- Specialty Expansion
- Treatment Locations
To respond to the surge of patients, hospitals had to deploy a tremendous amount of flexibility. As telehealth models expanded and improved access to specialists, increased coverage and navigated rapidly changing patient volumes. TeleHospitalists provided support for onsite staff as hospitals reached capacity and clinical teams were working longer hours to care for coronavirus patients.
The greater demand for healthcare also opened minds about how telemedicine can improve access to specialties where providers are not usually available. Suddenly, hospitals in rural communities unable to transfer ICU patients and needed direct, immediate support from infectious disease (ID), critical care and pulmonology physicians. While Eagle has been providing ICU and ID coverage for some time, few other telemedicine providers offered these specialties. The unique situation will hopefully expand care for the long term.
Finally, necessity is the mother of invention. After adopting more telemedicine care, hospitals and clinicians suddenly saw new places where telemedicine could improve the speed and quality of care.
The pandemic forced us all to quickly find ways to get care to patients. Telehealth providers customized delivery models to meet the immediate need and became more flexible as hospital requirements changed.
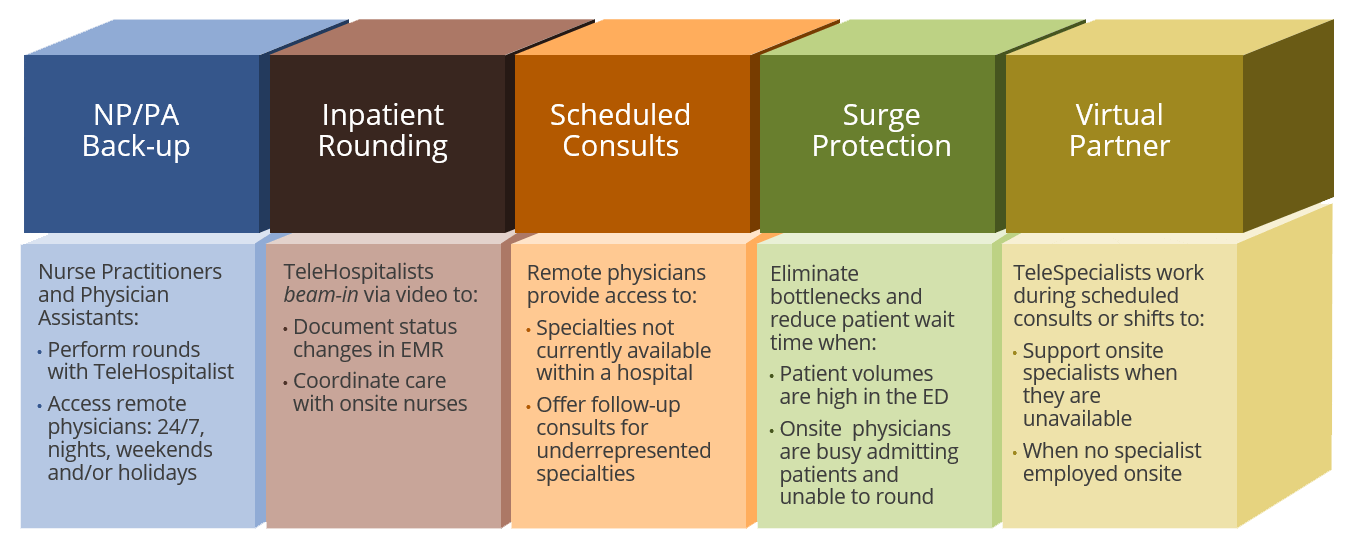
Common Synchronous Telemedicine Models:
Advanced Practitioner Back-up was particularly important when doctors prioritized caring for COVID patients. NPs and PAs were able to turn to TeleHospitalists to provide care for those patients in the hospital for other conditions. Our TeleIntensivists also supported APs working the ICU – managing ventilators and oxygen treatment.
Inpatient Rounding is part of the care TeleHospitalist and TeleIntensivists deliver remotely. The telemedicine providers beam-in to check on patients during the night. Remote physicians coordinate rounds with the nursing staff just as an onsite hospitalist would. Eagle doctors are also available to respond to changes in patient status. Nurses can request support at night without waking a physician that works during the day. If a patient’s vitals change, a virtual physician can complete an examination, provide a diagnosis and outline a treatment plan. In addition, Eagle physicians take calls to authorize less critical patient needs, like medication changes.
Scheduled Consults typically involve specialists, like TeleCardiologists, TelePulmonologists or TeleNeurologists. For example, a patient with an irregular heartbeat may see a TeleNocturnist who recommends a consult with a cardiologist. If there is no cardiologist onsite, a nurse can request a consult with a scheduled TeleCardiologist.
As more and more COVID patients arrived in the ED, Surge Protection became a more common solution. Surge protection provides access to remote physicians when patient volumes suddenly increase. Onsite physicians in the ED and on patient floors are busy admitting new patients or providing care to the most critical patients. That’s when a TeleHospitalist or Specialist will jump in and address the needs of patients that can receive a diagnosis from a remote physician. This was particularly important when Critical Access Hospitals were unable to transfer patients because of a surge in COVID patients at tertiary hospitals. This delivery model helps facilities respond quickly when there is an unexpected number of patients requiring care.
The Virtual Partner delivery model supports onsite care by providing all or almost all of the diagnosis and treatment plans in a particular specialty. This delivery model is most common in areas that don’t have a Neurologist or Nephrologist or even a Cardiologist onsite every day, all day. In these situations, Eagle partners with the hospital to provide access. The physician shortage has made this model more popular during 2020. In some facilities, Eagle asks as a virtual partner model to support a hospital with an on-site specialist to expand coverage during nights, weekends and vacations.
And, since a shortage of physicians is not going to disappear after we get the coronavirus under control, we expect this delivery model will continue to be popular in the future.
Eagle continues to be on the forefront by launching new specialties. Often, we add specialties in response to requests from hospitals we already work with. That’s how we grew from an organization focused on TeleHospitalist care in 2008 to offering 14 specialties today.
Before COVID many locations utilized TeleHospitalist, TeleNeurology, TelePsychiatry and TeleStroke coverage. Additionally, Eagle had Tele-ICU and Tele-ID programs in a several locations. COVID increased the need for all of these solutions.
So what changed? After the first wave of COVID patients subsided, hospitals started seeking new telemedicine applications, like:
- TeleCardiology
- Tele-GI
- TeleNephrology
- And, TelePulmonology
The interest in TelePulmonology is driven both by follow-up care for COVID patients and an overall rise in the need for pulmonology consults to treat pneumonia, COPD and other respiratory conditions.
What will we see in the future? As leaders in the industry, this is always top of mind. Eagle already offers Tele-MFM, TeleOncology and TelePediatrics. However, these programs are not adopted as frequently as other specialties. We expect this to change soon – in fact, Eagle just launched 2 new TeleOncology programs in Q1.
We also predict that high-resolution cameras will further enable remote wound care diagnosis and treatment. While remote physicians do not physically have hands on the patient, wound care physicians can provide specialized expertise when it comes to diagnosis. This expertise improves the treatment that patients receive from the physicians and advanced practitioners that are onsite.
WHITEPAPER: Strategies and Tips to Reduce Readmission

Here is the exciting part. COVID-19 did open minds about where remote care can help patients. We’ve talked to some organizations about access to synchronous telemedicine during patient transport. We haven’t yet deployed telemedicine during EMS or patient transfer. However, access to a remote physician for cardiac or stroke patients seems like a potential area where telemedicine could improve care.
Our Specialists are already working in Emergency Departments across the country but now they are doing it in new ways. Here is where the Surge Protection delivery model is a real game changer for hospitals with staffing issues.
TeleIntensivists provide support to onsite providers with everything, including high patient volume and patient status changes, as well as ventilator management and rounding. COVID expanded the need for coverage in this specialty. Unfortunately, Critical Care physicians already have very high burnout and turnover rates. Telemedicine can help reduce the stress to your onsite team by acting as a virtual partner to cover nights, holidays and weekends.
Hospitals with daytime physicians providing on-call coverage on nights and weekends quickly realized during 2020 that this model is unstainable. Nurses are often reluctant to wake a physician for less critical concerns. For those issues that require calling the doctor, the physician is tired when they take the call and often unrested when they arrive at work the next day.
TeleHospitalists and Specialists solve this problem because they are already awake and ready to go. In addition, hospitals that have trouble recruiting nocturnists, which is more and more common, often find telemedicine to be a logistic and cost-effective solution.
Coverage for outpatient clinics is a relatively new area for Eagle. Yet, the physician shortage and the pandemic combined to make outpatient follow-up service an important addition to our telemedicine offerings. Hospitals without a local specialist, particularly those in rural areas, can have the same Specialist provide inpatient or emergency department care to patients after they are discharged. These follow-up appointments are critical to monitoring patients and the appointments help hospitals lower readmission rates by making sure patients get access to the follow-up care they need in their community. Convenient care close to home makes all the difference to patients living 100 miles away from the nearest major metropolitan area.
As more and more Americans get vaccinated, we expect many of the telemedicine programs deployed during the pandemic will transition to serving long-term patient needs. After more than a year of struggle and loss, it’s heartening to know that some good will result from 2020. We predict that telehealth and synchronous telemedicine services will continue to expand – providing more access to specialists for patients everywhere.






